CE Expiration Date:
CEU (Continuing Education Unit): Credit(s)
AGD Code:
Educational aims and objectives
This clinical article aims to show how a new hydroxyapatite root repair material benefits the apical closure and healing of a large periradicular radiolucency.
Expected outcomes
Endodontic Practice US subscribers can answer the CE questions by taking the quiz to earn 2 hours of CE from reading this article. Correctly answering the questions will demonstrate the reader can:
- Consider the potential of iRoot® BP through the success of a case study.
- Realize some statistics regarding traumatic injuries to the upper incisors.
- Realize several options for treatment choices, carrying various risks for this patient.
- Observe the technique for removal of old root filling material for this patient.
- Observe canal disinfection, canal shaping, and management of the open apex for this patient.
Dr. Jason Bedford shares lessons learned about treating infected roots and hydroxyapatite root repair in his CE. Earn 2 CE credits after taking the quiz!
Dr. Jason Bedford shows how a new hydroxyapatite root repair material benefits the apical closure and healing of a large periradicular radiolucency
Introduction
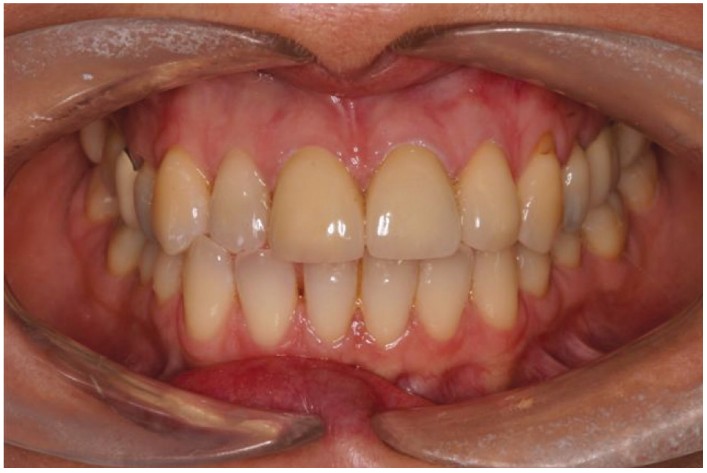
Traumatic injuries to the upper central incisors are extremely common. By the age of 20, 23% of males and 13% of females have suffered some degree of traumatic injury to their anterior teeth (Andreasen and Andreasen, 2000). These injuries are likely to take place between the ages of 8 and 10. At this age, many of the teeth injured are therefore immature, which complicates their management and long-term prognosis (Figure 1).

Contemporary endodontic techniques revolve around maintaining the vitality of the pulp, to encourage it to develop, and the root and pulp space to mature. In one study, over 50% of patients attending a pediatric dentistry clinic with complex enamel or dentin fractures were successfully treated using simple etch and bonding techniques with no need for root treatment (Cem Gungor, et al., 2007).
However, many older patients will not have had the benefit of these contemporary techniques. They will regularly present for treatment decades after the traumatic incident, requesting an esthetic improvement to their aging restorations. Unfortunately, these teeth often have longstanding, commonly asymptomatic endodontic infections, immature root formation, and large posts in situ. It is not unusual for patients to find it difficult to relate their presenting complaints with traumatic incidents that may have occurred decades earlier, of which they have very little recollection.
Managing these cases is not straight-forward, and the results can be unpredictable. Fortunately though, several options are now available to clinicians and their patients.
Case study
A 42-year-old woman was referred by her GDP for the assessment of the prognosis of two endodontically involved failing anterior crowns. The patient was fit and well, with no relevant medical history. Her main complaint was that one of her crowns had recently fractured and was currently replaced with a temporary crown. She was also concerned about discoloration of the tooth and the composite fillings in her other front teeth.
The teeth in question had originally been root-filled and crowned soon after they were damaged in a bicycle accident when the patient was approximately 10 years old. The crowns had been replaced several times over the years, and the current crowns had been in place for 15 years. The patient had not experienced any pain recently, but had been aware of a swelling below her upper lip for as long as she could remember.
On examination, the dentition was heavily restored but well cared for. There was a palpable swelling over the apices of the upper left incisor teeth. A small sinus was found adjacent to the upper left lateral incisor.
The upper left central incisor had been recently restored with a temporary crown. The lateral incisor had an all-ceramic crown, through which an access cavity had been made some years ago.

There were several composite restorations on the other anterior teeth that had begun to show their age, and the patient was keen to have replaced. X-rays of the anterior teeth revealed that the upper right central incisor had been root-filled some months before and had been asymptomatic since that time. There was some evidence of an apical radiolucency, which it was decided would be reviewed as it had only recently been completed.
The upper left central incisor had been restored with a wide, serrated metal post. The root-filling material had been placed to the correct apical extent, but appeared to be a single cone that did not completely obturate the canal. The tooth appeared to have an immature, open apex.
The upper left lateral incisor had been root-filled more recently. It looked well condensed but possibly 1 mm – 2 mm short of the radiographic root terminus. A large, well-circumscribed circular radiolucency, approximately 12 mm in diameter, appeared to be associated with the apices of both upper left incisors. Both teeth had lost the normal periodontal ligament space.
An initial diagnosis of failing root fillings UL1, UL2 with chronic periapical periodontitis was made. The alternative diagnoses of a root fracture UL1 or periradicular cyst were also considered (Figure 2). The treatment choices were:
- Orthograde revision of the root fillings
- Apical surgery
- Extraction followed by implant placement, a denture, or conventional bridge work

Option one: orthograde re-root fillings
Orthograde revision of the root fillings was complicated by several things:
- the presence of the large metal post in the UL1 — removal of this post was not without risk and could have resulted in a fracture of the root
- the extent of the apical lesion
- the long duration of the infection
- the immature/open apex present UL1
Additionally, even if successful, the end result for the UL1 would be a replacement post crown, of which 61% will last less than 10 years (Peutzfeld, et al., 2007).
Option two: apical surgery
One of the key indications for apical surgery is that there should be an adequate root filling in situ. Therefore, apical surgery was not indicated in this case. The patient was advised, however, that should the infection not respond to conventional endodontics, then apical surgery may be required.
Option three: extraction and replacement of UL1 and UL2
The opinion of an experienced implantologist was sought. After considering the practical difficulties posed by the large bony defect, the possible need for a bone graft and the cost implications, the patient decided against pursuing the implant option. The use of a bridge to replace the UL1 and UL2 was considered a last option by the patient. As implants were not appropriate, and a bridge could always be placed at a later date if the endodontic treatment failed, the patient asked us to attempt to revise the failing root fillings.
Conventional re-root filling is then broken down into several stages, all of which are relatively straightforward, but put together can result in a very long appointment.

Crown and post removal
The temporary crown was removed easily and the post removed using a combination of ET25 (Acteon) and CPR post removing ultrasonic tips (Dentsply Sirona).
Removal of old root filling material
The original root filling in the UR1 consisted of a single GP cone with sealer. This point was removed using a braiding technique. Three size 15 Hedstrom files are passed down either side of the GP cone. These are then twisted around each other, gripping the GP point. The files are then withdrawn together with the GP point.
The root filling material in the UR2 was more densely compacted. This was removed using the gutta-percha removal files — GPR files. These are used in a crown-down manner removing the GP down to the apical third. Often the GP cones will wrap around these files and are rapidly removed in one piece. If this is not the case, then the apical GP is softened with products such as orange solvent and removed manually with Hedstrom files.
Canal shaping
The UR1 required very little in the way of further canal preparation. The walls of the canal were debrided of residual filling materials using hand files. The apical diameter was gauged at size 80.
Canal disinfection
Careful irrigation with warmed 4% sodium hypochlorite solution was carried out throughout the shaping procedure. This was followed by a 1-minute rinse with 17% EDTA solution to remove any further debris and to dissolve the smear layer created during canal preparation.
The canal was then irrigated with more sodium hypochlorite, activated with Acteon Irrisafe™ ultrasonic tips (QED UK) (Figure 3). These have been shown to heat the irrigant and enhance its chemical and physical action on the bacterial biofilm present within the canal (Haappsalo, et al., 2010). The canals were then dressed with non-setting calcium hydroxide paste for 2 weeks.
Managing the open apex
At the second visit, the buccal swelling that had been present for months had resolved, and the area was much healthier looking. The patient reported that the discomfort had settled almost immediately following the first visit. The root canals were re-irrigated and dried using paper points. The apex of the central incisor was gauged to be around a size 80. This is too wide to be predictably obturated using traditional thermoplastic obturation techniques due to the risk of extrusion of the filling material into the apical tissues.
In recent years, apical-closure techniques have been described that utilize tricalcium phosphate cements, such as MTA. However, the mixing, manipulation, and placement of these materials can be frustratingly difficult. The use of hydroxyapatite to repair roots has long been established (Alhadainy, et al., 1998). Recently, pre-filled syringes of hydroxyapatite have become available in the form of iRoot® BP (Veriodent Canada) (Figure 3). The premixed material is relatively viscous and can simply be syringed into the canal. These products are considerably less expensive than MTA preparations.
The working length is marked on the syringe using a rubber stop and a small amount of the paste placed at the apex of the tooth. The needle is withdrawn as the paste is extruded, and the canal filled to the required depth. This is usually 4 mm – 5 mm.
The rest of the canal can be filled with gutta percha or in this case, a small amount of glass ionomer was place over the IRoot BP and a post space prepared. A temporary post crown was constructed, and the patient referred back to her general dental practitioner for the immediate construction of new anterior crowns.
3-month review stage
Although the patient had been asymptomatic, it was considered prudent to take a radiograph in order to assess the healing of the very large apical area at the 3-month stage (Figure 4). A periapical radiograph revealed rapid healing of the apical area. On closer examination, it also appears to show the formation of a hard tissue barrier apical to the hydroxyapatite paste (Figure 5).

The use of injectable hydroxyapatite paste such as iRoot BP provides a convenient, cost-effective, and predictable method of sealing canals with large apical diameters. This versatile material can also be used as a replacement for MTA in perforations, apicectomies, and pulp capping.
This article also considers hydroxyapatite root repair as an important part of treatment of furcation perforation. Read about it here and get 2 credits after taking the quiz! https://endopracticeus.com/ce-articles/furcation-perforation-current-approaches-and-future-perspectives/
References
- Alhadainy, HA, Himel, VT, Lee WB, Elbaghdady YM. The use of a Hydroxyapatite-based material and calcium sulfate as artificial floors to repair furcal perforations. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998;86(6):723-729.
- Andreasen JO, Andreasen FM. Essentials of Traumatic Injuries to the Teeth. 2nd ed. Copenhagen, Denmark: Munksgaard and Mosby; 2000,
- Cem Gungor H, Uysal S, Altay N. A retrospective evaluation of crown-fractured permanent teeth treated in a pediatric dentistry clinic, Dent Traumatol. 2007;23(4):211-217.
- Haapasalo M, Shen Ya, Oian W, Gao Y. Irrigation in endodontics. Dent Clin North Am. 2010;54(2):291-312.
- Peutzfeldt A, Sahafi A, Asmussen E. A survey of failed post-retained restorations. Clin Oral Investig. 2008;12(1):37-44.
Stay Relevant With Endodontic Practice US
Join our email list for CE courses and webinars, articles and more..


