Editor’s intro: This study delves into the adhesive strength of certain fiberglass posts with the use of different irrigation solutions.
Drs. Tiago André Fontoura de Melo and Daniel Galafassi, along with Cláudia Wagner, Bruna Machado dos Passos, and Priscila Souza de Souza, analyze the influence of an intracanal irrigating solution
Abstract
 This study aims to analyze the influence of the intracanal irrigating solution on the adhesive strength of cemented intraradicular fiberglass posts with RelyX™ U200. Sixty bovine lower incisors were randomly divided into six experimental groups according to the irrigation solution used in the mechanical chemical preparation: CN – saline, CP – saline + EDTA, CLX – 2% chlorhexidine digluconate, CLXE – 2% chlorhexidine digluconate + EDTA, HIP – 2.5% sodium hypochlorite, and HIPE – 2.5% sodium hypochlorite + EDTA. The root canals were filled with AH Plus®. After 72 hours in the greenhouse, the teeth were unthreaded to receive the fiberglass post cemented with RelyXTM U200. The samples were then sectioned in 1 mm according to the root thirds and subjected to the push-out test. After the test, the fractured samples were analyzed in a 20X stereomicroscope to determine the type of fracture. The obtained data was treated by the ANOVA two-way test, followed by the Tukey test. The non-parametric Kruskal-Wallis test was used to analyze the fracture type. The level of significance was 5%. There was a significant difference between irrigation solutions only in the middle-third of the root canal. In the association of saline solution with EDTA, there was a higher adhesion strength when compared to chlorhexidine and sodium hypochlorite associated with EDTA. The predominant type of failure was adhesive, with no difference between the different irrigation solutions.
This study aims to analyze the influence of the intracanal irrigating solution on the adhesive strength of cemented intraradicular fiberglass posts with RelyX™ U200. Sixty bovine lower incisors were randomly divided into six experimental groups according to the irrigation solution used in the mechanical chemical preparation: CN – saline, CP – saline + EDTA, CLX – 2% chlorhexidine digluconate, CLXE – 2% chlorhexidine digluconate + EDTA, HIP – 2.5% sodium hypochlorite, and HIPE – 2.5% sodium hypochlorite + EDTA. The root canals were filled with AH Plus®. After 72 hours in the greenhouse, the teeth were unthreaded to receive the fiberglass post cemented with RelyXTM U200. The samples were then sectioned in 1 mm according to the root thirds and subjected to the push-out test. After the test, the fractured samples were analyzed in a 20X stereomicroscope to determine the type of fracture. The obtained data was treated by the ANOVA two-way test, followed by the Tukey test. The non-parametric Kruskal-Wallis test was used to analyze the fracture type. The level of significance was 5%. There was a significant difference between irrigation solutions only in the middle-third of the root canal. In the association of saline solution with EDTA, there was a higher adhesion strength when compared to chlorhexidine and sodium hypochlorite associated with EDTA. The predominant type of failure was adhesive, with no difference between the different irrigation solutions.
Introduction
The use of prefabricated posts in the rehabilitation procedure of endodontically treated teeth has been widely used in dentistry (Castro, et al., 2012). The use of fiberglass posts has provided a better distribution of masticatory loads when compared to metal posts because their modulus of elasticity is very similar to that of dentin tissue (Newman, et al., 2003).
However, one factor much discussed in the literature is the stability and longevity of these esthetic posts. Several factors may be related to the failure of intraradicular material retention, such as the adhesive system and cement used and the type of dentin treatment performed before cementation (Cecchin, et al., 2011; Pereira, et al., 2013).
The adhesives and cements available in the market are very varied, and each material, depending on the composition and properties, may respond differently to endodontic treatments (Oliveira, et al., 2007). Therefore, it is important to analyze the changes that they can cause in the adhesion of the posts in the dentin. The adhesion strength tested in obturations was dissimilarly affected when using different irrigation solutions (Hashem, et al., 2009). Depending on the type of irrigation solution used during mechanical chemical preparation, a change in the adhesion of the post to the intraradicular dentin may occur.
The sodium hypochlorite solution decomposes in sodium chloride and oxygen, and this oxygen can inhibit the polymerization of resin cement and dentin adhesive (Nikaido, et al., 1999), as well as to promote the formation of bubbles that may interfere with resin infiltration within dentinal tubules (Ari, et al., 2003). Chlorhexidine digluconate does not dissolve organic components (Dametto, et al., 2005) and therefore may not facilitate the entry of the adhesive monomer into the dentinal tubules. Also, because of its adsorption characteristics, chlorhexidine digluconate may influence the adhesion strength of cemented posts in the root canal.
Thus, the purpose of this study is to analyze, by means of a mechanical push-out test, the influence of the type of intracanal irrigating solution on the adhesion of cemented intraradicular glass fiber posts with RelyXTM U200. The null hypothesis is that none of the irrigating solutions will influence the union force.
Methods
Selection and preparation of samples
Sixty bovine lower incisors intact and with complete rhizogenesis were selected, with the initial apical diameter of the root canal standardized with an endodontic instrument K-type No. 40 (Dentsply/Maillefer Instruments S.A., Ballaigues, Switzerland).
The dental crowns were sectioned at the cementoenamel junction, with the aid of diamond discs (American Burrs, Porto Alegre, Rio Grande do Sul, Brazil), in low rotation and under refrigeration. The length of the root remainder was standardized at 17 mm, and the working length (WL) was 1 mm below this measurement (WL = 16 mm).
Division of experimental groups
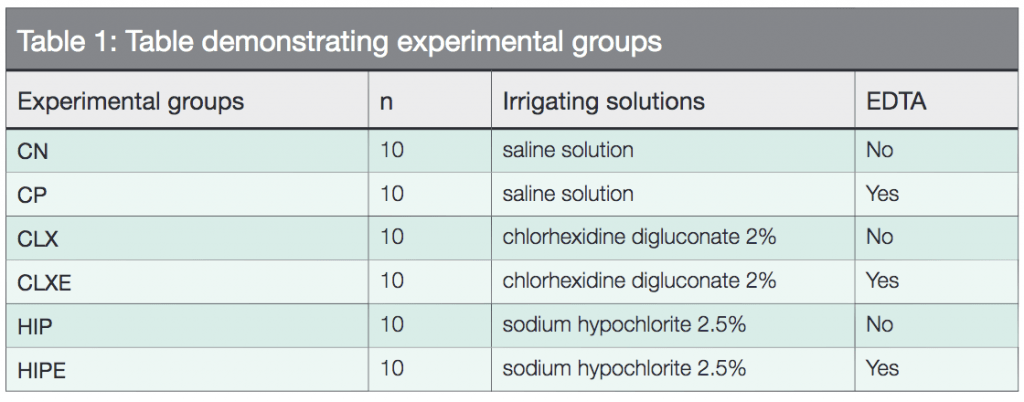
Samples were randomly divided into six experimental groups according to Table 1.
Endodontic treatment of the samples
All samples were manually prepared by the crown-apex technique with first- and second-series K-type stainless steel endodontic instruments (Dentsply/Maillefer Instruments S.A., Ballaigues, Switzerland). The diameter of the apical preparation was standardized with the use of instrument No. 60 in WL.
At each instrument change, the canals were irrigated with a plastic syringe (BD Solumed, São Paulo, São Paulo, Brazil) and NaviTip 25 mm 30ga needles (Ultradent, Indaiatuba, São Paulo, Brazil; South Jordan, Utah) with 2 mL of 2.5% sodium hypochlorite (Iodontec Indústria e Comércio de Produtos Odontológicos Ltda., Porto Alegre, Rio Grande do Sul, Brazil).
After the preparation, the final disinfection with filling of the root canal with 17% EDTA (Biodinamica, Ibiporã, Paraná, Brazil) was carried out under shaking of instrument No. 60 for 3 minutes. The canals were then irrigated with 2 mL of saline solution (Farmax, Divinópolis, Minas Gerais, Brazil) and dried with sterile absorbent paper tips No. 60 (Dentsply/Maillefer Instruments S.A., Ballaigues, Switzerland).
No intracanal medications were placed inside the canals; the samples were filled using AH Plus® cement (Dentsply/Maillefer Instruments S.A., Ballaigues, Switzerland) and the Tagger Hybrid Technique. The endodontic cement was proportioned and spatulated according to the manufacturer’s recommendations, and then the main tips of gutta percha No. 60 (Dentsply/Maillefer Instruments S.A., Ballaigues, Switzerland) were wrapped in cement and introduced into the WL. After insertion of the fifth accessory tip (Dentsply/Maillefer Instruments SA, Ballaigues, Switzerland) with the aid of the bidigital spacer B (Dentsply/Maillefer Instruments SA, Ballaigues, Switzerland), during lateral condensation, gutta-percha tips were plasticized by means of a McSpadden® No. 60 (Dentsply/Maillefer Instruments S.A., Ballaigues, Switzerland) calibrated at 4 mm below the WL, in order to obturate the middle and cervical thirds of the canal. After the gut plastification, the vertical condensation of the material was carried out with the aid of the Paiva No. 2 (S.S. White, Rio de Janeiro, Rio de Janeiro, Brazil; Lakewood, New Jersey).
The samples were provisionally restored to the cervical third with Cavit® (Septodont, Pomerode, Santa Catarina, Brazil; Lancaster, Pennsylvania) and remained immersed in a bottle containing distilled water (Iodontec Indústria e Comércio de Produtos Odontológicos Ltda., Porto Alegre, Rio Grande do Sul, Brazil) in an oven at 37 °C and 100% relative humidity for 2 days to ensure the complete setting of the endodontic cement.
Re-preparation of the canal and cementation of the fiberglass post
The canals were re-prepared using a DC2 drill (Whitepost, FGM, Joinville, Santa Catarina, Brazil) at a depth of 12 mm, with 4 mm of the obturator material remaining in the apical third.
Before cementation of the fiberglass posts, the canals were irrigated with 2.5% sodium hypochlorite solution and dried with absorbent paper tips, as recommended by the adhesive cement manufacturer.
With the dry canal, saline (FGM Produtos Odontológicos, Joinville, Santa Catarina, Brazil) was applied and dried at room temperature followed by application of air jets at a distance of 15 cm for 1 minute. The resinous cement RelyX™ U200 (3M/ESPE, Saint Paul, Minnesota) was applied to the root canal using a centrix syringe (DFL, Rio de Janeiro, Rio de Janeiro, Brazil) with a metal tip. The post was introduced into the root canal and filled with cement to the coronal portion to seal well the entrance and photoactivation with the aid of EC450 (ECEL, Ribeirão Preto, São Paulo, Brazil) for 40 seconds (20 seconds on each face: vestibular and lingual). The fiberglass posts used in the experiment were No. 2 (Angelus, Londrina, Paraná, Brazil). They were cleaned prior to use with alcohol 70 (Icarai, São Paulo, São Paulo, Brazil).
The samples were stored in distilled water for 48 hours to ensure the setting of the resin cement.

Shear extrusion test (push-out)
The samples were sectioned perpendicular to the long axis of the root with a diamond disk (American Burrs, Porto Alegre, Rio Grande do Sul, Brazil) in low rotation under refrigeration. A first cervical portion, approximately 1 mm thick, was discarded, as inherent imperfections in the adhesive zone, due mainly to the presence of oxygen, may influence the results (Van Noort, et al., 1991). Then three slices of approximately 1 mm thickness were obtained, one of the cervical third, one of the middle-third, and the other of the apical third. After cutting each slice, markings with an overhead pen were made on the cervical surface of the sample in order to highlight this face for later positioning of the piece at the time of the test. Then during the push-out test, each sample was placed on a metal device with a central opening larger than the canal diameter. The slices always remained with the cervical side down, facilitating the extrusion of the canal post/cement, which already presented with a conical shape, thus leaving the part of larger diameter down.
For the push-out test, an adapted metal cylinder (Ø = 1 mm) induced loading on the central portion of the post/cement, without the load being applied to the dentin (Figure 1).
The test was performed in a universal test machine (Instron® EMIC, São José dos Piñhais, Paraná, Brazil; Instron® Worldwide Headquarters, Norwood, Massachusetts) with a velocity of 0.5 mm/min and a load of 50 N (newton). The results were recorded in Newton and later converted to Mpa (Megapascal). The adhesion area (A) was calculated by the formula (2πr) multiplied by the height (L). The force (F) that occurred the fault were recorded in N and converted to Mpa. The adhesive resistance to the push-out was measured by dividing the force (F) by the adhesion area (A).
Analysis of fracture type
 After the push-out test, the fractured samples were stained with 7% hematoxylin for 3 minutes and analyzed in X20 stereo-
After the push-out test, the fractured samples were stained with 7% hematoxylin for 3 minutes and analyzed in X20 stereo-
microscope (Stemi 2000, Carl Zeiss, Germany; Carl Zeiss Meditec, Inc., Dublin, California) with a 50-fold increase in fracture type determination:
- Cohesive on the dental substrate — fracture predominantly (about 75%) within the dental structure
- Cohesive in the cement — fracture predominantly (about 75%) inside the cement
- Adhesive — fracture at the adhesive interface/dental structure or adhesive/cement interface in more than 75% of the analyzed area
- Mixed — fractures with no predominance greater than 75% of any type of failure (Le Bell, et al., 2004)
Statistical analysis
The obtained data was tabulated and submitted to two-way ANOVA followed by Tukey’s test, for multiple comparisons. The non-parametric Kruskal-Wallis test was used to analyze the fracture type. The level of significance was 5% (P ≤ 0.05). Statistical analysis was performed using SPSS 13.0 software (SPSS Inc., Chicago, Illinois).
Results
The mean values of the adhesion strength values (Mpa) of the different experimental groups in the different regions of the canal are shown in Table 2.
Means followed by distinct uppercase letters in the column and averages followed by different lowercase letters in the row differ significantly by means of the two-way ANOVA followed by Tukey’s test at a significance level of 5%.
The ANOVA two-way test, followed by the Tukey’s test, showed a significant statistical difference between the positive control group (CP) and the CLXE and HIPE groups (P = 0.021) only in the middle-third of the root canal.
When analyzing the experimental groups by root thirds, a significant statistical difference was observed between the cervical third in relation to the middle and apical for the CN, CLX CLXE, and HIP experimental groups (P <0.05).
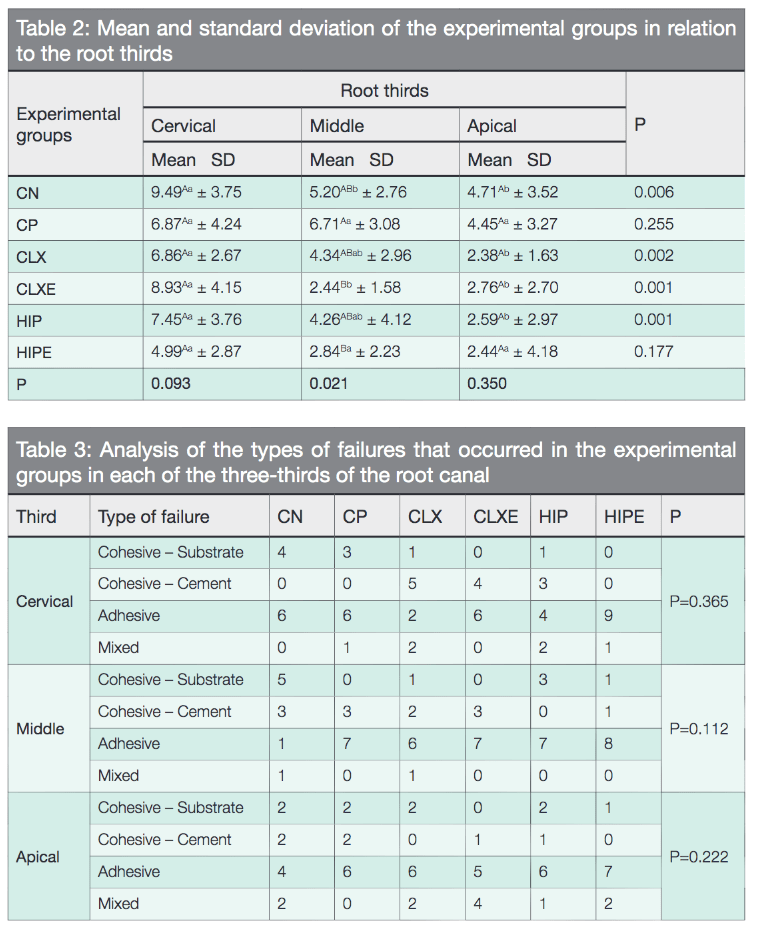
For analysis of the fracture type (Table 3), it can be observed that, although the predominant pattern of defects was adhesive, there was no difference between the groups tested in relation to the three-thirds root.
Discussion
According to Ari, et al. (2003), the type of irrigation solution used in the mechanical preparation of the root canal can cause deleterious effects on the bonding of the adhesive agents to the dentin structures. Therefore, the present study seeks to analyze if the type of endodontic irrigator influences the adhesion strength of intracanal cemented prefabricated posts.
Considering the irrigating solutions, it was decided to analyze 2.5% sodium hypochlorite and 2% chlorhexidine digluconate because they are the most used in endodontic treatment. The choice of physiological saline for use in the control groups is that it is an inert substance and does not present chemical action on the dentin tissues (Camilotti, et al., 2013).
As in other studies, canal obturation was performed shortly after mechanical chemical preparation to simulate endodontic treatment in a single session (Topcu, et al., 2010) and to avoid the influence of calcium hydroxide (Cohen, et al., 2002), used as intracanal medication.
According to Dimitrouli, et al. (2011), another factor that may also negatively influence the adhesive strength of glass fiber posts is the composition of certain endodontic cements. The cement of choice for the obturation of the study samples was based on epoxy resin AH Plus® because according to Kurtz, et al. (2003), this cement does not change the adhesive strength in the cementation process.
As in the study by Kirmali, et al. (2017), the use of the push-out test is a widely used feature in laboratory research to evaluate multiple factors that may influence intraradicular post retention. Another important detail is that, according to Goracci, et al. (2004), the push-out test represents the clinical situation better.
Initially, in the analysis of the results of the study, it can be observed that the type of irrigating solution influenced the adhesion strength of the intraradicular cemented glass fiber post in its middle-third, thus rejecting the null hypothesis presented in the objective.
In the analysis of irrigation solutions tested, associated or not to EDTA, it can be observed that there was a difference of adhesion to cementation of the post only in the middle-third of the canal. In the cervical and apical thirds, the behavior was equal between the groups. For Ozturk and Ozer (2004) and Arisu, et al. (2002), the use of intracanal sodium hypochlorite adversely affects the bond strength of resin cement, significantly reducing the modulus of elasticity of dentin (Marending, et al., 2007). Furthermore, because sodium hypochlorite dissociates in sodium chloride and oxygen, nascent oxygen can cause a strong inhibition of polymerization at the cementation interface (Greenstein, et al., 1986). In the study by Marques, et al. (2014), it can be observed that the use of 2.5% sodium hypochlorite significantly reduced adhesion strength, while the 2% chlorhexidine digluconate had no effect, as in Leitune, et al. (2010), and Lindblad, et al. (2010).
The adhesion of the dentin-resin interface can be compromised by degradation of the adhesive system components due to water absorption and/or proteolytic degradation of the hybrid layer, which is related to the action of metalloproteinases (Cecchin, et al., 2011) and cysteines cathepsin (Tersariol, et al., 2010). Some studies address the inhibition power of matrix metalloproteinases (MMPs) by chlorhexidine (Gendron, et al., 1999). For Brackett, et al. (2009), this inhibitory capacity may prevent the degradation of the relevant smear layer in dentin adhesion. In 2010, Topcu, et al. found that chlorhexidine digluconate favored adhesive resistance when compared to sodium hypochlorite and serum. However, in our study, no influence was observed on adhesion strength when chlorhexidine was used as an irrigant, associated or not with the use of EDTA 17%, in relation to the other irrigants tested.
One of the results in the data that drew attention was a lower adhesion strength obtained in the groups that made the association of the irrigant with the EDTA, although without significant difference on some occasions. This may be justified in some ways, since EDTA, as well as chlorhexidine, is also an inhibitor of MMPs (Faria and Silva, et al., 2013). In addition, the type of resin cement used in our study (RelyX™ U200), because it is self-adhesive, has a high potential of chemical reaction with dentin and may have its adhesion capacity impaired by the presence of demineralized apatite in the dentin caused by chelating action of EDTA itself.
Other data presented by some experimental groups (CN, CLX, CLXE, and HIP) and that generated reflection was that the force of adhesion in the cervical third of the canal was greater than in the middle and apical thirds. This finding was also observed in the study by Miguel Almeida, et al. (2012). It is believed that this result is not directly related to the type of irrigant tested, but rather to the fact that the photopolymerization of the cement in the cervical third is more effective than in the deep thirds of the root canal, which provides an increase in the adhesive resistance in this region (Hiraishi, et al., 2005). In addition, we also have the distribution and density of dentinal tubules in the different thirds of the root canal that can be correlated to this situation. The tubule density is higher in the cervical third than in the apical region of the root canal, and the tubule diameter decreases apically (Ferrari, et al., 2000). These anatomical variabilities suggest a greater adhesion near the cervical region (Topcu, et al., 2010).
Although there was no difference between the different irrigation solutions tested, the failures observed after the push-out test were predominantly adhesive. These results are consistent with other studies such as that of Bitter, et al. (2013) and Kirmah, et al. (2017), who observed the same fracture pattern.
Conclusions
According to the results, it can be concluded that, for the cervical and apical thirds, the irrigation solutions did not alter the adhesion process in the cementation of fiberglass posts. The EDTA-associated saline promoted a greater adhesion strength. The type of failure in the predominant fracture process was of adhesive origin.
After reading this study of different irrigation solutions, check out Dr. Jeffrey Krupp’s article “Endodontic irrigation involving the NaOCl component” for a look at different irrigation components in conjunction with the use of NaOCl.
- Ari H, Yasar E, Belli S. Effects of NaOCl on bond strengths of resin cements to root canal dentin. J Endod. 2003;29(4):248-251.
- Arisu HD, Kivanç BH, Sağlam BC, Şimşek E, Görgül G. Effect of post-space treatments on the push-out bond strength and failure modes of glass fibre posts. Aust Endod J. 2013;39(1):19-24.
- Bitter K, Hambarayan A, Neumann K, Blunck U, Sterzenbach G. Various irrigation protocols for final rinse to improve bond strengths of fiber posts inside the root canal. Eur J Oral Sci. 2013;121(4):349-354.
- Brackett MG, Tay FR, Brackett WW, et al. In vivo chlorhexidine stabilization of hybrid layers of an acetone-based dentin adhesive. Oper Dent. 2009;34(4):379-383.
- Camilotti V, Ioris MD, Busato PMR, Ueda K, Mendonça MJ. Evaluation of influence of irrigation solution in strength adhesive of a resin cement. Rev Odontol UNESP. 2013;42(2):83-88.
- Castro CG, Santana FR, Roscoe MG, et al. Fracture resistance and mode of failure of various types of root filled teeth. Int Endod J. 2012;45(9):840-847.
- Cecchin D, de Almeida JF, Gomes BP, Zaia AA, Ferraz CC. Influence of chlorhexidine and ethanol on the bond strength and durability of the adhesion of the fiber posts to root dentin using a total etching adhesive system. J Endod.2011;37(9):1310-1315.
- Cohen BI, Volovich Y, Musikant BL, Deutsch AS. The effects of eugenol and epoxy-resin on the strength of a hybrid composite resin. J Endod. 2002;28(2):79-82.
- Dametto FR, Ferraz CC, Gomes BP, et al. In vitro assessment of the immediate and prolonged antimicrobial action of chlorhexidine gel as an endodontic irrigant against Enterococcus faecalis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;99(6):768-772.
- Dimitrouli M, Günay H, Geurtsen W, Lührs AK. Push-out strength of fiber posts depending on the type of root canal filling and resin cement. Clin Oral Investig. 2011; 15(2):273-281.
- Faria e Silva AL, Menezes MS, Silva FP, Reis GR, Moraes RR. Intra-radicular dentin treatments and retention of fiber posts with self-adhesive resin cements. Braz Oral Res. 2013;27(1):14-19.
- Ferrari M, Mannocci F, Vichi A, Cagidiaco MC, Mjör IA. Bonding to root canal: structural characteristics of the substrate. Am J Dent. 2000;13(5):255-260.
- Gendron R, Grenier D, Sorsa T, Mayrand D. Inhibition of the activities of matrix metalloproteinases 2, 8, and 9 by chlorhexidine. Clin Diagn Lab Immunol. 1999;6(3):437-439.
- Goracci C, Tavares AU, Fabianelli A, et al. The adhesion between fiber posts and root canal walls: comparison between microtensile and push-out bond strength measurements. Eur J Oral Sci. 2004;112(4):353-361.
- Greenstein G, Berman C, Jaffin R. Chlorhexidine. An adjunct to periodontal therapy. J Periodontol. 1986;57(6):370-377.
- Hashem AA, Ghoneim AG, Lutfy RA, Fouda MY. The effect of different solutions on bond strength of two root canal-filling systems. J Endod. 2009;35(4):537-540.
- Hiraishi N, Papacchini F, Loushine RJ, et al. Shear bond strength of Resilon to a methacrylate-based root canal sealer. Int Endod J. 2005;38(10):753-763.
- Kırmalı Ö, Üstün Ö, Kapdan A, Kuştarcı A. Evaluation of various pretreatments to fiber post on the push-out bond strength of root canal dentin. J Endod.2017;43(7):1180-1185.
- Kurtz JS, Perdigão J, Geraldeli S, Hodges JS, Bowles WR. Bond strengths of tooth-colored posts, effect of sealer, dentin adhesive, and root region. Am J Dent. 2003;16(Spec No):31A-36A.
- Le Bell AM, Tanner J, Lassila LV, Kangasniemi I, Vallittu P. Bonding of composite resin luting cement to fiber-reinforced composite root canal posts. J Adhes Dent. 2004;6(4):319-325.
- Leitune VC, Collares FM, Werner Samuel SM. Influence of chlorhexidine application at longitudinal push-out bond strength of fiber posts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;110(5):77-81.
- Lindblad RM, Lassila LV, Salo V, Vallittu PK, Tjäderhane L. Effect of chlorhexidine on initial adhesion of fiber-reinforced post to root canal. J Dent. 2010;38(10):796-801.
- Marending M, Luder HU, Brunner TJ, et al. Effect of sodium hypochlorite on human root dentine — mechanical, chemical and structural evaluation. Int Endod J. 2007;40(10):786-793.
- Marques EF, Bueno CE, Veloso HH, Almeida G, Pinheiro SL. Influence of instrumentation techniques and irrigating solutions on bond strength of glass fiber posts to root dentin. Gen Dent.2014;62(2):50-53.
- Miguel-Almeida ME, Azevedo ML, Rached-Júnior FA, et al. Effect of light-activation with different light-curing units and time intervals on resin cement bond strength to intraradicular dentin. Braz Dent J. 2012;23(4):362-366.
- Newman MP, Yaman P, Dennison J, Rafter M, Billy E. Fracture resistance of endodontically treated teeth restored with composite post. J Prosthet Dent. 2003;89(4):360-367.
- Nikaido T, Takano Y, Sasafuchi Y, Burrow MF, Tagami J. Bond strengths to endodontically-treated teeth. Am J Dent. 1999;12(4):177-180.
- Oliveira LD, Carvalho CA, Nunes W, et al. Effects of chlorhexidine and sodium hypochlorite on the microhardness of root canal dentin. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;104(4):125-128.
- Ozturk B, Ozer F. Effect of NaOCl on bond strengths of bonding agents to pulp chamber lateral walls. J Endod. 2004;30(5):362-365.
- Pereira JR, Lins do Valle A, Ghizoni JS, et al. Push-out bond strengths of different dental cements used to cement glass fiber posts. J Prosthet Dent.2013;110(2):134-140.
- Tersariol IL, Geraldeli S, Minciotti CL, et al. Cysteine cathepsins in human dentin-pulp complex. J Endod. 2010;36(3):475-481.
- Topcu FT, Erdemir U, Sahinkesen G, Mumcu E, Yildiz E, Uslan I. Push-out bond strengths of two fiber post types bonded with different dentin bonding agents. J Biomed Mater Res B Appl Biomater. 2012;100(5):1458. <RETRACTED ARTICLE>
- Van Noort R, Cardew GE, Howard IC, Noroozi S. The effect of local interfacial geometry on the measurement of the tensile bond strength to dentin. J Dent Res.1991;70(5):889-893.
Stay Relevant With Endodontic Practice US
Join our email list for CE courses and webinars, articles and more..

