Dr. Bradley Trattner takes a conservative approach to save a tooth
Endodontic-periodontal lesions are complex entities that can be quite challenging. Diagnoses can be misleading and are often elusive. Determining whether the lesions are primarily endodontic, periodontal, or a combination of both can be difficult, and can affect the treatment plan and ultimately the success of any therapy as well. This can become the proverbial “chicken or the egg?” Which one came first, and which should we treat? Determining the prognoses can be equally vexing. With the current alternative of implants, some practitioners have been quick to “rush to judgment” and condemn a good number of teeth that can be saved. The following case is intended to give insight into and even possibly make us question some of our decision-making before we condemn a suspected endo-perio involved tooth.
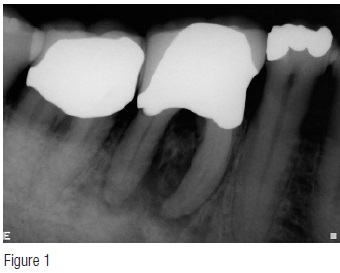
 A healthy, 65-year-old male presented with pain and swelling in the lower left quadrant. Clinical examination revealed a swelling in the buccal vestibule adjacent to tooth No. 30 that was tender to palpation and percussion. Cold vitality testing revealed normal responses from teeth Nos. 29 and 31 with no response obtained from tooth No. 30. His periodontal evaluation showed localized deep probing depths in the furcation area of tooth No. 30 ranging from 6 mm to 9 mm. Radiographic evaluation revealed severe bone loss in the furcation area with periapical radiolucencies developing around both the mesial and distal roots. A preliminary diagnosis of necrotic pulp secondary to periodontal involvement with an acute apical abscess was made.
A healthy, 65-year-old male presented with pain and swelling in the lower left quadrant. Clinical examination revealed a swelling in the buccal vestibule adjacent to tooth No. 30 that was tender to palpation and percussion. Cold vitality testing revealed normal responses from teeth Nos. 29 and 31 with no response obtained from tooth No. 30. His periodontal evaluation showed localized deep probing depths in the furcation area of tooth No. 30 ranging from 6 mm to 9 mm. Radiographic evaluation revealed severe bone loss in the furcation area with periapical radiolucencies developing around both the mesial and distal roots. A preliminary diagnosis of necrotic pulp secondary to periodontal involvement with an acute apical abscess was made.
Options of extraction and replacement with either an implant or bridge were discussed as well as endodontic treatment followed by periodontal intervention (usually guided tissue-regenerative procedures). The prognosis was discussed, and the patient was informed of a guarded (at best) outcome for endodontic treatment followed by periodontal intervention due to the severe bone loss in the furcation region. His general dentist and periodontist were consulted over the phone during the discussion. The patient made his intentions very clear; he wanted to save his tooth at all costs.
Tooth No. 30 was isolated with a rubber dam, and the necrotic pulp was accessed through the crown. After refining the access cavity, all canals (mesiobuccal, mesiolingual, and distal) were located, and the working lengths were determined using an apex locator and confirmed by X-ray. All canals were hand instrumented to the apex with a size 20 hand file and thereafter instrumented using EndoSequence® .04 files (Brasseler USA) to a master apical size of 30 on the mesial canals and size 35 on the distal canal. The canals were copiously irrigated with 6.25% sodium hypochlorite and subsequently dried with paper points. All canals were obturated using EndoSequence® BC Sealer™ and .04 BC Gutta Percha (Brasseler USA) utilizing a Synchronized Hydraulic Condensation Technique. The pulp chamber was explored internally throughout the procedure using a surgical microscope, and no internal fractures or anomalies were observed. The access cavity was closed using a sterile sponge and cavit. The patient was referred back to his general dentist for a permanent restoration of the access opening and to his periodontist for appropriate periodontal therapy.

 Needless to say, successful treatment of endo-perio lesions requires successful outcomes in both the endodontic and periodontal component of treatment. Successful endodontic treatment is based not only on the absence of periapical pathology but upon the long-term retention and function of the treated tooth. To that end, minimally invasive endodontic shaping can aid in this effort by preserving the maximum amount of radicular tooth structure, and thus, the structural integrity of the endodontically treated tooth. With the recent advent of bonded bioceramic cements (BC Sealer), hydraulic condensation, and enhanced irrigation techniques, we are able to conserve tooth structure and remove the critical biofilm and necrotic debris present in the canal(s). This can be accomplished by using .04 taper rotary files to prepare a constant tapered preparation that will preserve tooth structure and produce the desired shape (both EndoSequence and ESX® File Systems).
Needless to say, successful treatment of endo-perio lesions requires successful outcomes in both the endodontic and periodontal component of treatment. Successful endodontic treatment is based not only on the absence of periapical pathology but upon the long-term retention and function of the treated tooth. To that end, minimally invasive endodontic shaping can aid in this effort by preserving the maximum amount of radicular tooth structure, and thus, the structural integrity of the endodontically treated tooth. With the recent advent of bonded bioceramic cements (BC Sealer), hydraulic condensation, and enhanced irrigation techniques, we are able to conserve tooth structure and remove the critical biofilm and necrotic debris present in the canal(s). This can be accomplished by using .04 taper rotary files to prepare a constant tapered preparation that will preserve tooth structure and produce the desired shape (both EndoSequence and ESX® File Systems).
Successful periodontal treatment requires removal of all etiologic causative factors in the periodontal disease process retaining enough bone support and gingival health for tooth retention. During this case (as previously related), the patient was referred back to his general dentist for his permanent restoration and to a periodontist for periodontal treatment. As sometimes happens, this patient never followed up on his subsequent periodontal treatment, despite his insistence on saving his tooth at all costs. He returned for a 2-year follow-up radiograph with our office and had almost a complete regeneration of bone into the furcation area. His periodontal status was extremely good with probing depths on tooth No. 30 ranging 3mm to 4 mm with pink and healthy-appearing gingival tissue. Note: The contralateral molar (No. 19) has had a type II furcation that has been stable for the last few years. The fact that his periodontal condition had healed with only endodontic treatment preformed on this tooth would indicate that the initial diagnosis of necrotic pulp secondary to periodontal involvement with an acute apical abscess was incorrect. A correct diagnosis of a primary endodontic lesion with secondary periodontal involvement would be more accurate. Complete elimination of the contaminated pulp (the primary etiology) was after the fact, all that was necessary to provide the environment for this apparent combined lesion to heal.
More than likely, I would not have treated this tooth if it had not been for the insistence of the patient. Kim in 2008 found a significantly lower endodontic success rate in teeth with endo-perio lesions. A study in 2006 performed at the University of Minnesota by Doyle and Hodges found that restored endodontically treated teeth and single-tooth implant restorations had similar failure rates, although the implant group showed a longer average and median time to function and had a higher incidence of postoperative complications requiring subsequent treatment intervention. In 2013, Levin found that implant survival rates do not exceed those of compromised but adequately treated and maintained teeth; supporting the notion that the decision to extract a tooth and place an implant should be made cautiously. Many practitioners are quick to “rush to judgment” in this implant-dominated world in which we live. Maybe we should start to listen to our patients more often and err (if we are to) on the side of being conservative and trying to save more teeth.
References
1. Kim E, Song JS, Jung IY, Lee SJ, Kim S. Prospective clinical study evaluating endodontic microsurgery outcomes for cases with lesions of endodontic origin compared with cases with lesions of combined periodontal-endodontic origin. J Endod. 2008;34(5):546–551.
2. Doyle SL, Hodges JS, Pesun IJ, Law AS, Bowles WR. Retrospective cross sectional comparison of initial nonsurgical endodontic treatment and single-tooth implants. J Endod. 2006;32(9):822-827.
3. Levin L, Halperin-Sternfeld M. Tooth preservation or implant placement: a systemic review of long-term tooth and implant survival rates. J Am Dent Assoc. 2013;144(10):1119-1133.
Stay Relevant With Endodontic Practice US
Join our email list for CE courses and webinars, articles and more..

