CE Expiration Date:
CEU (Continuing Education Unit): Credit(s)
AGD Code:
Educational aims and objectives
This article aims to present and discuss nonsurgical endodontic treatment of a maxillary central incisor diagnosed with infected dens invaginatus (Oehlers’ Type III) and associated apical periodontitis utilizing ultrasonic and hand instruments and the surgical operating microscope as an auxiliary tool for both diagnosis and treatment planning.
Expected outcomes
Endodontic Practice US subscribers can answer the CE questions by taking the quiz to earn 2 hours of CE from reading this article.
Take the quiz by clicking here.
Correctly answering the questions will demonstrate the reader can:
- Observe nonsurgical endodontic treatment of a maxillary central incisor diagnosed with infected dens invaginatus (Oehlers’ Type III) and associated apical periodontitis utilizing ultrasonic and hand instruments and the surgical operating microscope as an auxiliary tool for both diagnosis and treatment planning.
- Identify some etiology of dens invaginatus (DI).
- Identify some challenges of teeth with DI for root canal therapy because of their complex anatomy.
- Recognize the importance of a meticulous radiographic inspection for identification of DI, and the benefits of CBCT imaging in the diagnosis of teeth with unusual anatomy.
- Recognize the benefits of using an operating surgical microscope and ultrasonic instruments during these clinical procedures.
Drs. Jorge Vieyra and Fabian Acosta elaborate on a treatment for a patient with dens invaginatus
Drs. Jorge Vieyra and Fabian Acosta present a case report that describes the diagnosis and conservative treatment of a unilateral case of a maxillary central incisor with an infected Type III dens invaginatus and an associated periradicular lesion
Dens invaginatus (DI) is a growth-related malformation resulting from invagination of the crown before calcification has developed (Hüllsmann, 1997). As the hard tissues are created, the invaginated enamel organ creates a small tooth inside the forthcoming pulp chamber. In the severe type of dens invaginatus, there is a folding of Hertwig’s epithelial sheath into the developing root (Bhaskar, 1986).
The etiology of this dental malformation remains controversial, and although many hypotheses have been proposed, none has been supported or widely accepted. Numerous issues have been suggested to explain this uncommon dental formation, including trauma, infection, inhibition of the growth of specific cells, disruption of factors that regulate the formation of the enamel organ, and links to genetic factors (Hüllsmann, 1997; Alani and Bishop, 2008; Hosey and Bedi, 1996).
Salter described a radiographic image that seems to be “a tooth within tooth” (Salter, 1855). DI can be cataloged according to its complexity, with the well-documented classification of Oehlers (1957) describing three forms according to the complexity of the invagination into the root: Type I is limited to the crown, whereas Type II invagination extended inside the root, ending as a blind pod. Type III invagination invades the entire root and exit apically or laterally (Figure 1). Its occurrence varies from 0.3% to 10% (Hovland and Block, 1977), with the upper lateral incisor the most frequently affected tooth followed by the upper central incisor.
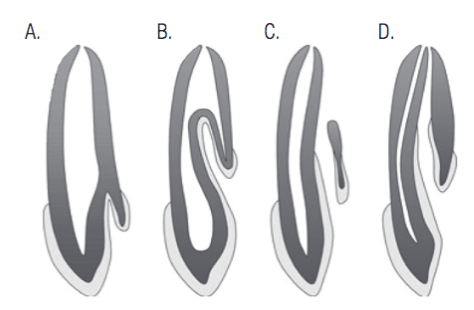
Teeth with DI pose a challenge for root canal therapy because of their complex anatomy. Numerous clinical procedures have been proposed such as nonsurgical root canal treatment (Hovland and Block, 1977), combined root canal and surgical treatment (Benenati, 1994), planned replantation (Lindner, et al., 1995), and extraction (Rotstein, et al., 1987). However, planned replantation and extraction are commonly the last decision. Outcome studies for the management of teeth with DI are, however, unavailable due to the rarity of the condition.
The following clinical circumstance describes the successful nonsurgical RCT of a maxillary central incisor diagnosed with infected dens invaginatus (Oehlers’ Type III) and associated apical periodontitis utilizing ultrasonic and hand instruments. Surgical operating microscopes were used as an aid for diagnosis, and the planning of treatment is highlighted.
Case report
A 22-year-old male patient presented at the dental school in Tijuana, Mexico, with a history of pain and inflammation in the maxillary right anterior region. After initial examination, the patient was referred to the endodontic department for consultation and further management. The patient reported mild pain and swelling about a week before, but at the day of examination, there were no clinical manifestations.
Diagnosis and treatment planning
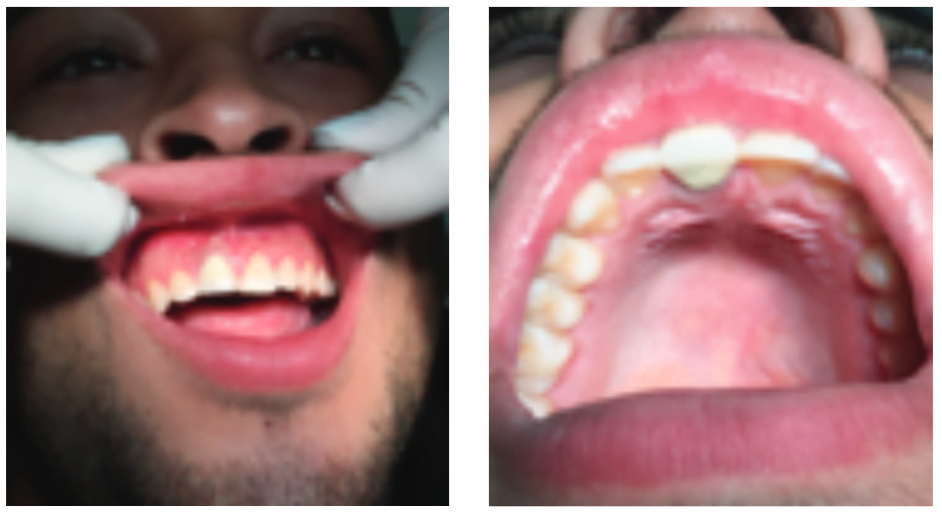
Clinical inspection showed the maxillary right central incisor UR1 restored with a porcelain crown. There was no sign of sinus tract or swelling; nonetheless, the tooth was vaguely tender to tapping. The labial mucosa related to the maxillary right central incisor was sore. The porcelain crown was removed, and UR1 was non-responsive to cold stimulation (Endo-Ice®, Coltene), while the adjacent teeth responded normally. A periodontal examining was within standard limits (Figures 2A and 2B).
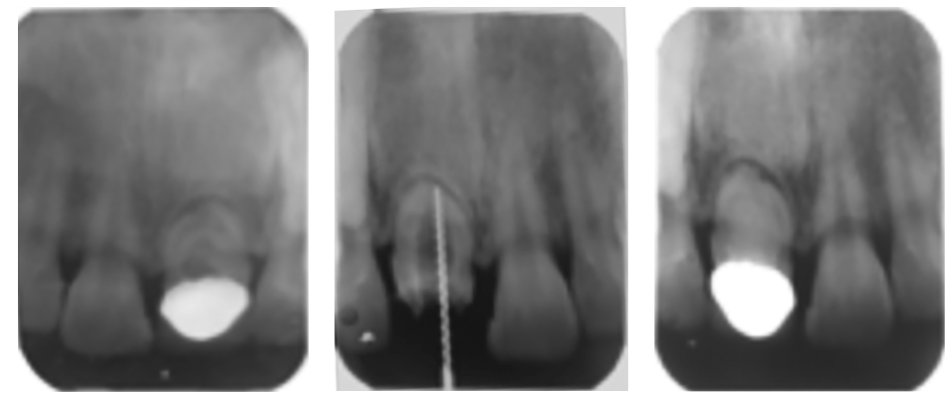
Radiographic inspection showed immature root development, an apical radiolucency of about 4 mm in diameter, and an abnormal internal structure corresponding with Type III DI (Figure 3A). A diagnosis of pulp necrosis with apical periodontitis was made. The contralateral central incisor was also tested for clinical and radiographic signs of the same malformation, but there were none.
The patient’s general dentist had suggested antibiotics (amoxicillin 250 mg, 3 times a day for 7 days) and an analgesic (ibuprofen 400 mg, 3 times a day for 7 days).
Treatment procedure
A clinical strategy was developed that included nonsurgical root canal treatment (RCT) of the dens tract over some appointments, comprising the use of a calcium hydroxide dressing. The treatment plan presented to, and accepted by, the patient was to perform removal of the DI and the infected necrotic pulp tissue, followed by the complete RCT. Written consent was obtained before initiation of RCT and notably addressed all the available treatment options and their associated risks, benefits, and challenges.
A surgical operating microscope (Carl Zeiss Surgical, Oberkochen, Germany) was used during the treatment. After anesthesia with 2% lidocaine, 1: 100,000 epinephrine (Xylocaine®, Dentsply Sirona), the crown was removed during diagnostic phase, and a rubber dam was placed and stabilized with dental dam cord (Wedjets®, Coltene). Access was prepared with a 331-carbide bur in the lingual side of the tooth.
Entrance into the large pulp chamber of the invagination via an occlusal access revealed a serosanguinous discharge, which could drain.
The infected pulp tissue was removed, and the irregular invaginated tissue was cautiously eliminated by chemomechanical preparation using ultrasonic endodontic tips sizes 2-4 (ProUltra® endo-coated instrument, Dentsply Sirona) at power setting 4 of the ultrasonic unit (Satelec P5, Acteon UK) in a brushing movement starting from an apical to coronal direction.
The root canal was prepared primarily with a long tapered diamond bur to improve access to the apical defect. Working length of the dens tract was estimated with an apex locator (Root ZX; J Morita Corp, Tustin, California) and was verified radiographically (Figure 3B).
The root canal was initially debrided with large K-file instruments up to size 90. The master apical size of 130 was achieved using K-files (SybronEndo, Orange, California). The remaining root canal was molded as far as possible with Gates Glidden drills (Dentsply Maillefer) sizes 2-4.
To maximize proper disinfection, irrigation was performed with 5.25% sodium hypochlorite (NaOCl) in the pulp chamber and 2.5% NaOCl in the apical part of the canal system with regard to incomplete apical closure of the root. Some 2 ml of 17% EDTA was used to remove the smear layer. The final irrigation of the canal with NaOCl was supported using the ultrasonic unit (Piezon Master 400; EMS, Optident UK). Sodium hypochlorite was delivered into the canal by using a syringe, and ultrasonic passive irrigation was performed for 1 minute.
The root canal was desiccated with sterile absorbent paper cones size #100, and dressed with Ca(OH)2 paste (Pulpdent Corp, Watertown, Massachusetts). The entrance of the pulp chamber was temporarily sealed with Cavit™ (3M Oral Care) and Fuji IX (GC UK) to avoid infection of the root canal system. The porcelain crown was cleaned and replaced for esthetic reasons (Figure 3C).
The patient returned after 2 weeks, having remained free of any symptoms. At this second appointment, the tooth was not sensitive to percussion, and the soft tissues in the area were not tender to palpation. The tooth was anesthetized as earlier defined, and a rubber dam was placed. The invagination was opened and flooded with 1% NaOCl followed by a final rinse with 17% EDTA for 1 minute and passive ultrasonic irrigation (ProUltra tips 1 and 2; Dentsply Maillefer, Ballaigues, Switzerland) with 1% sodium hypochlorite for 1 minute after elimination of calcium hydroxide paste.
After additional irrigation, the canal was desiccated with sterile absorbent paper cones, and further Ca(OH)2 was placed in the canal. The tooth was temporarily sealed with Cavit and Fuji IX as previously described. The patient was requested to return 3 weeks later for completion of nonsurgical RCT.
At the third visit, the tooth was anesthetized as described before and isolated with a rubber dam. The tooth was accessed, and Ca(OH)2 was removed from the root canal with passive ultrasonic irrigation, and the canal was desiccated with sterile absorbent paper cones size #100.
The prepared root canal was filled with a master apical gutta-percha cone size #110 (Figure 3D) and warm gutta percha using an Obtura gun (Obtura II, Fenton, Missouri) and AH26® sealer (DeTrey Dentsply, Konstanz, Germany). A bolus of thermoplasticized injectable gutta percha heated to 150 ºF, was delivered, carefully positioned around the master apical gutta percha with use of Schilder pluggers size No. 10 (Dentsply Maillefer, Ballaigues, Switzerland). Serial radiographs were exposed to visualize and check its acceptable adaptation and to confirm the absence of extrusion outside the apical foramen (Figure 3E). The rest of the root canal system was then filled with thermoplasticized gutta percha, warmed to 150 ºF.
The access was sealed with a light-cured composite, and a postoperative radiograph was taken. The patient was advised to take 400 mg ibuprofen (every 6 hours as needed for pain); antibiotics were not deemed necessary because of the absence of signs/symptoms. The patient was then referred to his attending dentist, and he was asked to return in 48 hours and was seen at 1-month, 3-month, 6-month and 1-year recall periods (Figure 3F).

Discussion
RCT of teeth with DI can be demanding because of the capricious form of the internal anatomy and the circumstance that the dens tract is covered with enamel (Hüllsmann, 1997). Additionally, pulp necrosis in such teeth usually develops before complete apical closure, leaving the root canal with a wide apical opening. The clinical protocol includes an effective treatment plan based on the knowledge of signs, symptoms, and radiographs. A meticulous radiographic inspection plays a key role in the identification of DI. Nevertheless, standard or digital periapical radiographs may not show the features and size of the invagination (Vier-Pelisser, et al., 2012). CBCT imaging has been shown to be useful in the diagnosis of teeth with unusual anatomy. The introduction of cone beam computed tomography (CBCT) brought about a revolution in dentistry that has contributed to the planning, diagnosis, therapy, and prognosis of several dental procedures (Kaneko, et al., 2011). Teeth with DI present physical defects that are predisposed to caries because of the deep pits, which act as locations of plaque retention.
Microbes and their products may exacerbate infection and lead to necrosis of the pulp, frequently before final maturation of the root (Cengiz, 2006). Therefore, DI requires early diagnosis and treatment. A major condition for effective RCT is the whole elimination of irritants from the infected root canal system.
A tooth with DI shows a diversity of canal morphologies such as concavities, intracanal communications, apical ramifications, and other regions that instruments cannot reach. The complicated structure in DI affects the prognosis of the tooth. The case of DI presented here exemplifies only one clinical handling approach, which may not necessarily be appropriate in all such clinical scenarios.
The irregular dimensions of the root canal system make proper shaping and cleaning complicated. A large amount of dentin has to be removed to ensure adequate cleaning. Regrettably, this may end in increased fracture predisposition of the thin root-end walls.
Elimination of the invaginated form of hard tissue in the root canal is tough and challenging. Thus, the clinician should select a suitable way to eliminate the hard tissue, the necrotic material, and the microorganisms. In this case, the use of an operating surgical microscope and ultrasonic instruments facilitated the clinical procedures. In some clinical situations, the abnormal structure of DI is internal and an independent unit from the rest of the tooth. In these occurrences, the complete elimination of the central-anomalous structure and total elimination of pulp tissue can be followed with this valuable clinical aid.
An ideal endodontic repair material should seal the pathways of communication between the root canal and its neighboring tissues. It should be harmless, non-carcinogenic, biocompatible, insoluble in tissue fluids, and physically stable (Bogen and Kuttler, 2009).
Calcium hydroxide as interappointment treatment, ultrasonic instrumentation, and passive irrigation are necessary and suggested (Bishop and Alani, 2008). Obturation techniques using thermoplasticized injection of gutta percha are proper for such teeth because they allow flow of softened gutta percha into unreachable areas better than other techniques, but they have a risk of extrusion in teeth with an open apex (de Sousa and Bramante, 1998).
Several methods have been proposed to strengthen the root (Katebzadeh, et al., 1998; Lertchirakarn, et al., 2002). Materials like MTA can be considered an option in RCT of immature permanent teeth with DI with the advantage of shorter treatment time, good sealing ability, and great biocompatibility (Kumar, et al., 2014).
The procedural difficulty encountered is controlling the overfill or underfill of MTA. Most of these include bonding a material to the root dentin inside the root canals. However, it has been shown that such a bond can break down over time (Kitasako, 2002).
Hence, long-term decrease of fracture exposure employing bonding techniques must be debatable. In the present-day case, the dentin wall seemed to be practically thick, so fracture was not a main concern (Brooks and Ribera, 2014; Narayana, et al., 2012; Zoya, et al., 2015; Zhang and Wei, 2017).
Conclusions
The present-day report shows the truthful diagnosis and conservative treatment of dens invaginatus using current endodontic methods. This case report demonstrates that Type III dens invaginatus can be treated nonsurgically with the aid of the dental operating microscope, and ultrasonic and hand endodontic instruments.
Check out how Dr. Garth used 3D imaging to diagnose a patient with dens invaginatus in his article, “Nonsurgical root canal therapy on a tooth with dens invaginatus.”
References
- Alani A, Bishop K. Dens invaginatus: Part 1: classification, prevalence and aetiology. Int Endod J. 2008; 41(12):1123-36.
- Benenati FW. Complex treatment of a maxillary lateral incisor with dens invaginatus and associated aberrant morphology. J Endod. 1994;20(4):180-182.
- Bhaskar SN. Synopsis of Oral Pathology. J Oral Maxillofac Surg. 1986;44(11):929
- Bishop K, Alani A. Dens invaginatus. Part 2: clinical, radiographic features and management options. Int Endod J. 2008;41(12):1137-1154.
- Bogen G, Kuttler S. Mineral trioxide aggregate obturation: a review and case series. J Endod. 2009; 35(6):777-790.
- Brooks JK, Ribera MJ. Successful nonsurgical endodontic outcome of a severely affected permanent maxillary canine with dens invaginatus Oehlers type 3. J Endod. 2014;40(10):1702-1707.
- Cengiz SB, Korasli D, Ziraman F, et al. Non-surgical root canal treatment of dens invaginatus: reports of three cases. Int Dent J. 2006;56(1):17-21.
- de Sousa SM, Bramante CM. Dens invaginatus: treatment choices. Endod Dent Traumatol. 1998; 14(4):152-158.
- Hosey MT, Bedi R. Multiple dens invaginatus in two brothers. Endod Dent Traumatol. 1996;12(1):44-47.
- Hüllsmann M. Dens invaginatus: aetiology, classification, prevalence, diagnosis, and treatment considerations. Int Endod J. 1997;30(2):79-90.
- Hovland EJ, Block RM. Nonrecognition and subsequent endodontic treatment of dens invaginatus. J Endod. 1977;3(9):360-362.
- Lindner C, Messer HH, Tyas MJ. A complex treatment of dens invaginatus. Endod Dent Traumatol. 1995;11(3):153-155.
- Kaneko T, Sakaue H, Okiji T, Suda H. Clinical management of dens invaginatus in a maxillary lateral incisor with the aid of cone-beam computed tomography—a case report. Dent Traumatol. 2011;27(6): 478-483.
- Katebzadeh N, Dalton BC, Trope M. Strengthening immature teeth during and after apexification. J Endod. 1998;4(24):256-259.
- Kitasako Y, Burrow MF, Nikaido T, Tagami J. Long-term tensile bond durability of two different 4-META containing resin cements to dentin. Dent Mater. 2002;18(3):276-280.
- Kumar A, Yadav A, Shetty N. One-step apexification using platelet rich fibrin matrix and mineral trioxide aggregate apical barrier. Indian J Dent Res. 2014;25(6):809-812.
- Lertchirakarn V, Timyam A, Messer HH. Effects of root canal sealers on vertical root fracture resistance of endodontically treated teeth. J Endod. 2002;28(3):217-219.
- Narayana P, Hartwell Wallace R, Nair UP. Endodontic Clinical Management of a Dens Invaginatus Case by Using a Unique Treatment Approach: A Case Report. J Endod. 2012;38(8):1145-1148.
- Oehlers FA. Dens invaginatus. I. Variations of the invagination process and associated anterior crown forms. Oral Surg Oral Med Oral Pathol. 1957;10(11):1204-2018.
- Rotstein I, Stabholz A, Heling I, Friedman S. Clinical considerations in the treatment of dens invaginatus. Endod Dent Traumatol. 1987;3(5):249-254.
- Salter S. Warty tooth. Trans Pathol Soc Lond. 1855;6:173-177.
- Vier-Pelisser FV, Pelisser A, Recuero LC, et al. Use of cone beam computed tomography in the diagnosis, planning and follow up of a type III dens invaginatus case. Int Endod J. 2012;45(42):198-208.
- Zhang P, Wei X. Combined Therapy for a Rare Case of Type III Dens Invaginatus in a Mandibular Central Incisor with a Periapical Lesion: A Case Report. J Endod. 2017;43(8):1378-1382.
- Zoya A, Ali S, Alam S, et al. Double Dens Invaginatus with Multiple Canals in a Maxillary Central Incisor: Retreatment and Managing Complications. Int Endod J. 2015;11:1927-1932.
- Vertucci FJ. Root canal anatomy. of the human permanent teeth. Oral Surg Oral Med Oral Pathol. 1984;58(5):589-599.
Stay Relevant With Endodontic Practice US
Join our email list for CE courses and webinars, articles and more..


