Drs. Mario Luis Zuolo and Arthur de Siqueira Zuolo present clinical detection, diagnosis, and management of a non-vital central incisor with an open apex
The treatment of immature necrotic teeth with non-vital pulps and open apices often presents a challenge to the clinician. Cleaning and shaping the thin canal walls, controlling the infection, and performing a satisfactory sealing of the apex sometimes are not possible.1 In most cases, the treatment involves the induction of apical closure by apexification procedures to allow more favorable conditions for the conventional treatment.
[userloggedin]
2
Traditionally, calcium hydroxide has been the material of choice used to induce the formation of an apical hard tissue barrier before placing the permanent filling.3 Although many studies have reported favorable outcomes when this treatment is followed,4-7 some disadvantages have also been reported. The use of calcium hydroxide apical barriers has been associated with some problems, such as unpredictability of apical closure,8 risk of re-infection due to leakage in the provisional fillings,9 and risk of root fracture as a result of the long-term application of calcium hydroxide.10-11 Furthermore, poor patient compliance also has a negative influence on the prognosis of traditional apexification procedures.12
With the advent of the mineral trioxide aggregate (MTA), a calcium silicate-based biocompatible non-absorbable material, another option of treatment has been proposed.13 This material has the ability to set in a short period of time and in the presence of moisture. It solidifies into a hard structure in less than 3 hours.14 This property, along with its capacity of inducing cementum-like hard tissue when used in the periradicular tissues,15 allows its use in the immediate obturation of open apex.16-18 Several studies show that apexification with MTA has a high success rate with less visits and in less time to completion.18-21 Also, in a study that compared clinical and radiographic results of apexification with MTA or calcium hydroxide, all of the cases sealed with MTA healed, whereas in the calcium hydroxide cases, two out of 15 remained with the disease.9
However, MTA also has some disadvantages. Because of its consistency, its manipulation and placement in the site of repair can be challenging.22 Additionally, its use can cause discoloration of the tooth, and it should be used with caution when in esthetic zones.23 A novel material MTA REPAIR HP — “High Plasticity” MTA (Angelus®, Londrina, PR, Brazil) was recently introduced with the intent to improve some of those characteristics.24 This new formula maintains all the chemical and biological properties of the original MTA; however, it changes its physical properties of manipulation, resulting in a greater plasticity, and therefore facilitating manipulation and insertion. Additionally, its formula uses a different radiopacifier calcium tungstate (CaW04) that, according to the manufacturer, does not cause staining of the root or dental crown.24
In this report, we present clinical detection, diagnosis, and management of a non-vital central incisor with an open apex, using a novel MTA-based repairing material.
Case report
A 12-year-old male patient with a noncontributory medical history presented for examination with chief complaint of pain in the tooth No. 11. Clinical examination showed that the tooth had been restored with a temporary filling and responded with pain to percussion and palpation and also presented a discrete edema in the area. There was no probing defect or sinus tract stoma. According to the patient, a root canal treatment had been started in the tooth approximately 12 months before. In the radiographic examination, a radiopaque material inside the canal a few millimeters short of the apex could be noticed. Also, in the radiograph, it could be seen that the apex was not completely formed and presented a periapical lesion (Figure 1). A clinical diagnosis of pulpless tooth with unsatisfactory previously initiated therapy and symptomatic apical periodontitis was established.

The treatment plan was to initially perform the cleaning and shaping of the canal and to place a calcium hydroxide dressing. Then after 1 to 2 weeks, with the regression of the symptoms, we would perform an apical barrier with a new MTA-based material, obturate the tooth, and restore it. The treatment plan was presented to the patient’s parents, who agreed to it.
After the consent form was signed, 1.8 mL of local anesthesia (lidocaine 2% with epinephrine 1:100.000) was administrated, the restoring material was removed, and endodontic access corrected. After rubber dam isolation, the material inside the canal was removed with proper irrigation using a 2.5% sodium hypochlorite solution (Formula e Ação, São Paulo, SP, Brazil) and a CPR-7® ultrasonic tip (Obtura Spartan® Endodontics, Algonquin, Illinois)
After the removal of the material in the canal, Largo burs (No. 2 and No. 3) were used to prepare the first two-thirds of the canal. Then the apical foramen was located with the aid of an apex locator (Raypex®, VDW, Munich, Germany), and working length (WL) was established at the “0.0” and confirmed with a radiograph. Instrumentation proceeded using stainless-steel K-type hand files in a crown-down technique until a size No. 80 hand file achieved the WL. Between each change of file, copious irrigation with 2.5% sodium hypochlorite solution was used as an irrigant (approximately 100 mL throughout the whole treatment). During the procedure, passive ultrasonic irrigation (PUI) was performed for 1 minute several times to assure complete removal of the prior material and to maximize the irrigation technique. After the completion of instrumentation, the canal was irrigated with 5 mL EDTA 17% (Formula e Ação, São Paulo, SP, Brazil) for 3 minutes and a final rinse with 5 mL saline solution. A calcium hydroxide-based paste was placed in the canal as an interappointment dressing, and the tooth was temporarily restored (Figure 2).

After 10 days, the patient came to the clinic to conclude treatment. The tooth was asymptomatic, and the area was no longer swollen. The temporary filling was removed, the calcium hydroxide paste was removed from the canal using 2.5% sodium hypo-chlorite solution, and PUI as described before. Hand file No. 80 was used again at WL. The canal was then irrigated with 5 mL of EDTA 17% (Formula e Ação, São Paulo, SP, Brazil) for 3 minutes to remove smear layer, and 5 mL of saline solution was used for final rinse. The canal was dried with paper points, and MTA HP (Angelus, Londrina, Brazil) was manipulated according to manufacturer instructions and placed with the aid of pluggers (B&L Biotech Inc., Fairfax, Virginia) in the last 3 mm of the root canal, forming an apical plug. After 10 minutes, the material was set, and the tooth was obturated using BC Sealer™ (Brasseler USA®, Savannah, Georgia) and gutta-percha cones with lateral condensation technique (Figure 3).
The pulp chamber was cleaned with a sponge soaked in 70% alcohol, and the access cavity was restored using composite (Figure 4). A high-resolution CBCT was requested to the patient immediately after treatment so it could be used for comparison later in the follow-up.
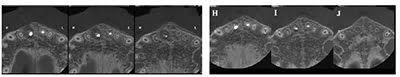
The patient presented for recall 1 month later without any symptoms. Postoperative radiographic and clinical evaluations were performed at 3, 6, and 9 months. The tooth was asymptomatic, and the area did not have any signs of inflammation. After 9 months, another tomographic exam was made. Comparison of the CBCT images was performed, and bone healing and apical closure of the open apex could be observed (Figures 4-5).
Discussion
Previous clinical studies in humans have demonstrated that an apical barrier of MTA can be used with success in the technique of apexification of teeth with open apices. El Meligy, et al., (2006), ran a clinical trial comparing the use of calcium hydroxide and MTA in 30 teeth of 15 patients who had lost pulp vitality by caries or trauma. The conventional technique of apexification with calcium hydroxide was performed in one tooth, whereas the barrier technique with MTA was applied to the other tooth in the same patient. The teeth were then followed up for 3, 6, and 12 months, revealing that two of the teeth filled using calcium hydroxide failed, while none of the teeth filled with MTA showed clinical or radiographic signs of pathology. Simon, et al., (2007), carried out a prospective clinical trial in 57 teeth of 50 patients with open apices treated with MTA plug and definitive filling of the canal and observed success in 81% of the cases.
In this case report, the use of a modified MTA (MTA-BIOCERAMICS-based high-plasticity reparative cement) has shown a good clinical result considering the short follow-up period observed. Comparison of tomographic images just after the placement of the MTA barrier and after a 9-month period has demonstrated bone formation and closure of the apical portion with hard tissue. It should be noted that a radiolucent area also could be seen at this time. Such pattern of healing could be classified as incomplete healing according to Molven, et al., (1996).
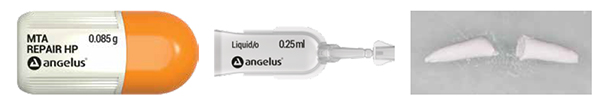
From a clinical point of view, the handling and placement of the MTA REPAIR HP was easier than the conventional MTA. According to the manufacturer, the difference is in the replacement of distilled water (from the conventional Angelus MTA) by a liquid that contains water and another organic plasticizer that gives the new product high plasticity24 (Figure 6). The other manufacturer claim that the new MTA does not promote dental discoloration could not be studied since the material was placed in the apical portion of the canal.
The importance of case reports is the demonstration of what is possible in our patients using scientific-based clinical protocols of treatment. Reports from clinical practitioners have played important roles in the field of dentistry but should be validated using adequate laboratory and clinical research studies. In conclusion, the clinical protocol using the new MTA REPAIR HP, described in this case report, enabled the successful apexification of a central incisor in a young patient.
[/userloggedin]
[userloggedout][/userloggedout]
- Trope M. Treatment of immature teeth with non-vital pulps and apical periodontitis. Endod Topics. 2006;14:51–59.
- Rafter M. Apexification: a review. Dent Traumatol. 2005;21(1):1-8.
- Granath LE. Some notes on the treatment of traumatized incisors in children. Odont Rev. 1959;10:272.
- Morfis AS, Siskos G. Apexification with the use of calcium hydroxide: a clinical study. J Clin Pediatr Dent. 1991;16(1):13–19.
- Kleier DJ, Barr ES. A study of endodontically apexified teeth. Endod Dent Traumatol. 1991;7(3):112–117.
- Walia T, Chawla HS, Gauba K. Management of wide open apices in non-vital permanent teeth with Ca(OH)2 paste. J Clin Pediatr Dent. 2000;25(1):51–56.
- Dominguez Reyes A, Munoz Munoz L, Aznar Martin T. Study of calcium hydroxide apexification in 26 young permanent incisors. Dent Traumatol. 2005;21(3):141-145.
- Sübay RK, Kayataş M. Dens invaginatus in an immature maxillary lateral incisor: a case report of complex endodontic treatment. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;102(2):e37-41.
- El-Meligy OA, Avery DR. Comparison of apexification with mineral trioxide aggregate and calcium hydroxide. Pediatr Dent. 2006;28(3):248-253.
- Andreasen JO, Farik B, Munksgaard EC. Long-term calcium hydroxide as a root canal dressing may increase risk of root fracture. Dent Traumatol. 2002;18(3):134–137.
- Andreasen JO, Munksgaard EC, Bakland LK. Comparison of fracture resistance in root canals of immature sheep teeth after filling with calcium hydroxide or MTA. Dent Traumatol. 2006;22(3):154–156.
- Heling I, Lustmann J, Hover R, Bichacho N. Complications of apexification resulting from poor patient compliance: report of case. ASDC J Dent Child. 1999;66(6):415–418.
- Torabinejad M, Chivian N. Clinical applications of mineral trioxide aggregate. J Endod. 1999;25(3):197–205.
- Torabinejad M, Hong CU, McDonald F, Pitt Ford TR. Physical and chemical properties of a new root-end filling material. J Endod. 1995;21(7):349–353.
- Shabahang S, Torabinejad M, Boyne PP, Abedi H, McMillan P. A comparative study of root-end induction using osteogenic protein-1, calcium hydroxide, and mineral trioxide aggregate in dogs. J Endod. 1999;25(1):1–5.
- Simon S, Rilliard F, Berdal A, Machtou P. The use of mineral trioxide aggregate in one-visit apexification treatment: a prospective study. Int Endod J. 2007;40(3):186–197.
- Steinig TH, Regan JD, Gutmann JL. The use and predictable placement of mineral trioxide aggregate in one-visit apexification cases. Aust Endod J. 2003;29(1):34–42.
- Witherspoon DE, Small JC, Regan JD, Nunn M. Retrospective analysis of open apex teeth obturated with mineral trioxide aggregate. J Endod. 2008;34(10):1171-1176.
- Mente J, Hage N, Pfefferle T, Koch MJ, Dreyhaupt J, Staehle HJ, Friedman S. Mineral trioxide aggregate apical plugs in teeth with open apical foramina: a retrospective analysis of treatment outcome. J Endod. 2009;35(10):1354–1358.
- Nayar S, Bishop K, Alani A. A report on the clinical and radiographic outcomes of 38 cases of apexification with mineral trioxide aggregate. Eur J Prosthodont Restor Dent. 2009;17(4):150–156.
- Holden DT, Schwartz SA, Kirkpatrick TC, Schindler WG. Clinical outcomes of artificial root-end barriers with mineral trioxide aggregate in teeth with immature apices. J Endod. 2008;34(7):812–817.
- Seltzer S, Sinai I, August D. Periodontal effects of root perforations before and during endodontic procedures. J Dent Res. 1970;49(2):332–339.
- de Chevigny , Dao TT, Basrani BR, Marquis V, Farzaneh M, Abitbol S, Friedman S. Treatment outcome in endodontics: the Toronto study — phases 3 and 4: orthograde retreatment. J Endod. 2008;34(2):131-137.
- Angelus. MTA REPAIR HP. https://angelus.ind.br/MTA-REPAIR-HP-292.html. Accessed April 4, 2016.
- Molven O, Halse A, Grung B. Incomplete healing (scar tissue) after periapical surgery — radiographic findings 8 to 12 years after treatment. J Endod. 1996;2(5):264-268.
MTA HP product is under FDA approval and will be launched in the US and Canada during 2016.
Stay Relevant With Endodontic Practice US
Join our email list for CE courses and webinars, articles and more..

 Mario Luis Zuolo, DDS, MSc, practices at Endodontic Specialists in Sao Paulo, Brazil. He has a Masters in Molecular Biology from UNIFESP-Paulista School of Medicine, Sao Paulo, Brazil, and is a Professor in the graduate department of Endodontics, Professor in the Endodontics Programming at EAP-APCD, Sao Paulo, Brazil. Dr. Zuolo lectures globally on endodontics. The author of numerous publications since 1998, most recently co-wrote Reintervention in Endodontics, published by Quintessence in 2014.
Mario Luis Zuolo, DDS, MSc, practices at Endodontic Specialists in Sao Paulo, Brazil. He has a Masters in Molecular Biology from UNIFESP-Paulista School of Medicine, Sao Paulo, Brazil, and is a Professor in the graduate department of Endodontics, Professor in the Endodontics Programming at EAP-APCD, Sao Paulo, Brazil. Dr. Zuolo lectures globally on endodontics. The author of numerous publications since 1998, most recently co-wrote Reintervention in Endodontics, published by Quintessence in 2014. Arthur de Siqueira Zuolo, DDS, MSc, graduated from the University of Sao Paulo (USP), Faculty of Dentistry in Ribeirão Preto, Brazil, in 2010. He has a postgraduate degree in Endodontics from New York University in New York and a Masters and Specialist in Endodontics by Faculty of Dentistry at São Leopoldo Mandic, Campinas, Brazil. Dr. Zuolo is also an Adjunct Professor of Endodontics Specialty at APCD, Sao Paulo, Brazil. He has a private practice in Sao Paulo, Brazil, and is a co-author of the book Reintervention in Endodontics, published by Quintessence in 2014.
Arthur de Siqueira Zuolo, DDS, MSc, graduated from the University of Sao Paulo (USP), Faculty of Dentistry in Ribeirão Preto, Brazil, in 2010. He has a postgraduate degree in Endodontics from New York University in New York and a Masters and Specialist in Endodontics by Faculty of Dentistry at São Leopoldo Mandic, Campinas, Brazil. Dr. Zuolo is also an Adjunct Professor of Endodontics Specialty at APCD, Sao Paulo, Brazil. He has a private practice in Sao Paulo, Brazil, and is a co-author of the book Reintervention in Endodontics, published by Quintessence in 2014.